Bacterial infections are a common health issue in dogs and can be caused by a variety of bacteria. These infections can affect different areas of the body, including the skin, ears, urinary tract, and kidneys.
Dogs can transmit several viral and bacterial diseases to humans, making it important to be aware of the types of bacterial infections that can affect them. In this article, we will discuss nine types of bacterial infections that commonly affect dogs, their symptoms, and treatment options.
You are reading: 9 Types Of Bacterial Infections In Dogs
9 Types Of Bacterial Infections In Dogs
Salmonella
Salmonella is a type of bacterial infection that can affect dogs. It is caused by the Salmonella spp bacteria, which is mainly an intestinal pathogen but can also cause systemic disease and can then be isolated from blood and various organs.
Salmonella infections are common in dogs worldwide, with the exception of the Nordic countries where the incidence is low. Dogs can become infected through contaminated food and contaminated water, and the feeding of raw meat is the most common route of transmission in dogs.
Salmonella infections are most common in dogs who have a compromised immune system, and puppies are more likely to develop salmonellosis. Symptoms of salmonella infection in dogs include fever, diarrhea, vomiting, lethargy, dehydration, loss of appetite, depression, and decreased activity.
Salmonella infections are uncommon in dogs and cats, but they can be carriers of the bacteria, which means that even if the pets don’t show symptoms of salmonellosis, they can still shed Salmonella in their stool and saliva and then spread the bacteria to the home environment and to people and other pets in the household.
If you suspect that your dog has a salmonella infection, it’s important to take them to the vet for proper diagnosis and treatment.
Leptospirosis
Leptospirosis is a bacterial infection that can have serious consequences in dogs and can also affect humans. It is caused by spiral-shaped bacteria called leptospires, which thrive in moist environments and in water.
Dogs can become infected by coming into contact with urine of infected animals, which can contaminate water, soil, and mud. The most common way dogs get leptospirosis is through water contaminated with urine, particularly stagnant or slow-moving water like puddles, ponds, or lakes.
Dogs can also contract leptospirosis through contact with urine-contaminated soil, bedding, or food, or by eating infected tissues or carcasses. Symptoms of leptospirosis in dogs vary and can include fever, vomiting, abdominal pain, diarrhea, refusal to eat, severe weakness and depression, stiffness, or severe muscle pain.
In severe cases, rapid or difficulty breathing may be noted from bleeding into the lung (pulmonary hemorrhage). Leptospirosis can cause kidney failure with or without liver failure, and affected dogs can also develop swollen legs or accumulate excess fluid in their chest or abdomen.
Leptospirosis is responsive to antibiotics, and complete recovery is possible, but some dogs that survive may be left with chronic kidney or liver disease.
Leptospirosis is a zoonotic disease, which means that it can be transmitted from dogs to humans. If you suspect that your dog has leptospirosis, it’s important to take them to the vet for proper diagnosis and treatment.
Staph Infection

Staphylococcus (staph) infections are the most commonly-seen bacterial skin problems in dogs. Staph infections are caused by the Staphylococcus spp bacteria, which are normally found in small numbers on the skin of all dogs.
However, if the skin becomes irritated or injured, the bacteria can invade the area and an infection can develop. Dogs with allergies or who have diseases that weaken the immune system, such as hypothyroidism or Cushing’s syndrome, for example, can develop infections in their skin and ears or their respiratory, reproductive, or urinary tracts, in addition to other areas.
Any dog can contract a staph infection, but puppies and senior dogs tend to have weaker immune systems and are more prone to them than healthy adult dogs.
Staph infections can also be transmitted from dog to dog, and from dogs to humans, although this is rare. Symptoms of staph infection in dogs include redness, inflammation, itchiness, head shaking, abnormal ear discharge, and crusts or scabs in the ears.
Treatment for staph infections in dogs typically involves antibiotics, and in severe cases, additional support such as fluids for dehydrated pets may be needed. Good hygiene practices, such as regular bathing and grooming, can help prevent staph infections in dogs.
Ear Infection
Read more : Why Is My Dog Licking My Other Dog?
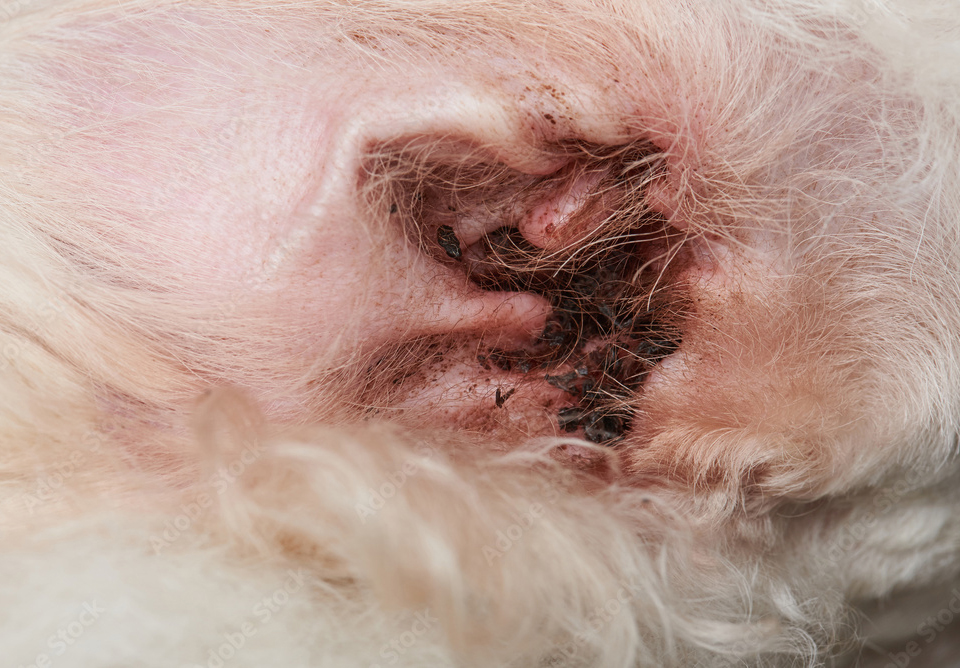
Ear infections are a common health issue in dogs and can be caused by a variety of factors, including bacteria, yeast, ear mites, foreign objects, allergies, and hormonal imbalances.
The canine ear canal is more vertical than that of a human, forming an L-shape that tends to hold in fluid, making dogs more prone to ear infections.
Symptoms of ear infections in dogs include swelling of the ear, head shaking or tilting, crusts or scabs just inside the ear, rubbing the ear on the floor or furniture, redness and swelling of the ear canal, pain, itchiness, and dark discharge with an odor. If left untreated, ear infections can lead to more serious complications, such as facial paralysis, balance and coordination issues, and severe pain.
Treatment for ear infections in dogs typically involves cleaning the ear thoroughly to remove debris, discharge, and ear wax, and the use of medicated ear cleaners or topical medications. In more severe cases, oral antibiotics or anti-inflammatory medications may be prescribed by a veterinarian.
Preventive measures, such as regular ear cleaning and grooming, can help reduce the risk of ear infections in dogs. If you suspect that your dog has an ear infection, it’s important to take them to the vet for proper diagnosis and treatment.
Actinomycosis
Actinomycosis is a rare chronic bacterial infection caused by Actinomyces spp., which are gram-positive filamentous non-acid fast anaerobic to microaerophilic bacteria that typically colonize the human mouth, urogenital tract, and gastrointestinal tract.
Actinomycosis is usually a granulomatous and suppurative infection that may involve multiple sulfur-containing abscesses that form sinus tracts. The chronic form of actinomycosis has multiple abscesses that form sinus tracts and are associated with sulfur granules.
Actinomycosis is generally not diagnosed until the chronic phase. Actinomycosis is usually caused by Actinomyces israelii, which is a common organism found in the nose and throat. Actinomycosis can affect different parts of the body, including the face, neck, abdomen, pelvis, and lungs.
Actinomycosis spreads slowly into nearby tissues, usually causing a long-lasting, tunneling wound (an opening underneath the skin) that is filled with yellowish pus and sulfur granules.
Actinomycosis is responsive to antibiotics, and treatment usually requires antibiotics for several months to a year. In more severe cases, surgical drainage or removal of the affected area (lesion) may be needed.
If you suspect that your dog has actinomycosis, it’s important to take them to the vet for proper diagnosis and treatment.
Streptococcus
Streptococcus is a genus of gram-positive bacteria that can cause a variety of infections in dogs and humans. There are several types of streptococcal bacteria, but the most common types that cause infections in people are group A and group B.
Group A streptococcus can cause strep throat, scarlet fever, impetigo, toxic shock syndrome, cellulitis, and necrotizing fasciitis (flesh-eating disease).
Group B streptococcus can cause blood infections, pneumonia, and meningitis in newborns, and urinary tract infections, blood infections, skin infections, and pneumonia in adults.
In dogs, streptococcal infections can cause skin infections, pneumonia, and meningitis. Streptococcal infections are usually treated with antibiotics, and in severe cases, hospitalization may be necessary.
To prevent streptococcal infections, it’s important to practice good hygiene, such as washing your hands regularly, covering your mouth and nose when coughing or sneezing, and avoiding close contact with people who are sick.
If you suspect that you or your dog has a streptococcal infection, it’s important to seek medical attention promptly.
Bordetella
Bordetella bronchiseptica is a bacterium that is associated with respiratory disease in dogs. It is one of the most common bacterial agents responsible for kennel cough in dogs.
Kennel cough is a highly contagious respiratory disease that can spread quickly in environments where dogs are in close proximity to each other, such as boarding kennels, dog daycare centers, shows, dog parks, and training classes.
The Bordetella vaccine is a non-core vaccine that can help prevent kennel cough in dogs that are frequently exposed to other dogs in social settings. The vaccine is usually given annually to healthy adult dogs that come into contact with large groups of other dogs, and boarding facilities may require a booster within the last six months.
Puppies should receive the injectable version of the Bordetella vaccine between the ages of six to eight weeks, followed by a second injectable booster four weeks later or between the ages of 10 to 12 weeks.
Read more : 12 Types Of Herding Dogs
Adult dogs should receive a booster form of the Bordetella vaccine every six to twelve months, depending on the risk factors for the dog. The Bordetella vaccine is an optional vaccine, not a core vaccine, and your veterinarian can help you determine whether this vaccine is appropriate for your dog.
E. coli
Escherichia coli (E. coli) is a type of bacteria that normally lives in the intestines of healthy people and animals. Most types of E. coli are harmless and even help keep your digestive tract healthy, but some strains can cause illness.
E. coli infections in dogs are rare, but they can occur. Dogs can become infected with E. coli by eating contaminated food or drinking contaminated water. Symptoms of E. coli infection in dogs include vomiting, diarrhea, and loss of appetite.
In severe cases, E. coli infection can lead to dehydration, kidney failure, and even death. Treatment for E. coli infection in dogs typically involves antibiotics and supportive care, such as fluids for dehydrated pets.
To prevent E. coli infection in dogs, it’s important to practice good hygiene, such as washing your hands regularly, cleaning up after your dog, and avoiding contact with other dogs that are sick.
In humans, E. coli infections can cause a range of symptoms, from mild diarrhea to severe illness and even death. E. coli infections in humans are usually caused by eating contaminated food, such as undercooked ground beef or raw vegetables, or by drinking contaminated water.
To prevent E. coli infection in humans, it’s important to practice good food safety, such as cooking meat thoroughly, washing fruits and vegetables, and avoiding cross-contamination in the kitchen.
Clostridia
Clostridia are a group of gram-positive, anaerobic bacteria that are widely distributed in the environment, including soil, dust, and vegetation, and are also part of the normal bacterial flora in the colon and vagina.
Most species of the genus Clostridium are saprophytic organisms that ferment plant polysaccharides and are found in many places in the environment, most notably the soil.
However, some species of Clostridium can cause serious infections in humans and animals, including gas gangrene, tetanus, botulism, pseudomembranous colitis, and food poisoning.
Clostridia infections are usually opportunistic, meaning that they establish a nidus of infection in a particular site in a compromised host. Clostridia infections can be diagnosed by recognizing the characteristics of the lesion of the infection along with Gram stains of the tissue and bacterial culture.
Treatment for Clostridia infections typically involves antibiotics and supportive care, such as fluids for dehydrated pets, and in some cases, tissue debridement or removal of the affected area (lesion) may be needed.
Clostridia bacteria are commonly found in the gut microbiome, and overuse of antibiotics can cause an imbalance of the gut microbiome, leading to overgrowth of the species Clostridioides difficile, causing a serious infection (CDI).
Clostridia infections of the abdomen and pelvis are serious and sometimes fatal, and Clostridia produce large amounts of gas, which can form bubbles and blisters in the infected tissue.
To prevent Clostridia infections, it’s important to practice good hygiene, such as washing your hands regularly, cleaning up after your pet, and avoiding contact with other pets that are sick.
FAQS
1. What are the most common types of bacterial infections in dogs?
The most common types of bacterial infections in dogs include salmonella, leptospirosis, staph infection, ear infection, actinomycosis, streptococcus, bordetella, E. coli, and clostridia.
2. How do dogs get bacterial infections?
Dogs can get bacterial infections through a variety of ways, including contaminated food and water, contact with other infected animals, and exposure to bacteria in the environment.
3. What are the symptoms of bacterial infections in dogs?
Symptoms of bacterial infections in dogs vary depending on the type of infection, but can include fever, vomiting, diarrhea, loss of appetite, lethargy, skin irritation, and respiratory problems.
4. How are bacterial infections in dogs treated?
Treatment for bacterial infections in dogs typically involves antibiotics and supportive care, such as fluids for dehydrated pets. In severe cases, hospitalization may be necessary.
5. Can bacterial infections in dogs be prevented?
Preventing bacterial infections in dogs involves practicing good hygiene, such as washing your hands regularly, cleaning up after your pet, and avoiding contact with other pets that are sick. Vaccines are also available for some types of bacterial infections, such as bordetella.
6. Can bacterial infections in dogs be transmitted to humans?
Yes, some types of bacterial infections in dogs can be transmitted to humans, so it’s important to practice good hygiene and seek medical attention if you suspect that you or your dog has a bacterial infection.
Source: https://petstutorial.com
Category: DOGS